Women’s Health Library
Our Health Library information does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their health. Our providers may not see and/or treat all topics found herein.
Prostate Cancer
Condition Basics
What is prostate cancer?
Prostate cancer is the abnormal growth of cells in the prostate gland. (The prostate is part of the male reproductive system. It is a small organ below the bladder that makes fluid for semen.)
Most cases of prostate cancer occur after age 65. It usually grows slowly and can take years to grow large enough to cause any problems.
In some cases, the cancer grows more quickly. It may spread within the prostate, to nearby lymph nodes and other tissues, and to other parts of the body. But usually prostate cancer is found early, before the cancer has spread outside the prostate.
What causes it?
Experts don't know exactly what causes prostate cancer. But they do know that changes in the body's DNA are involved. These include DNA changes that are inherited as well as those that happen as you get older.
What are the symptoms?
Prostate cancer usually doesn't cause symptoms in its early stages. When there are symptoms, they are most often problems with urinating. You may also have deep and frequent pain in your lower back, belly, hip, or pelvis.
How is it diagnosed?
Your doctor may check for prostate cancer with a blood test called a prostate-specific antigen (PSA) test. And you will probably have a digital rectal exam. If your PSA level is high, you'll likely have more tests to find the cause. A prostate biopsy is needed to confirm a diagnosis of prostate cancer.
How is prostate cancer treated?
Treatment for prostate cancer is based on the stage of the cancer, your Gleason score, and other things, such as your age and overall health. The main options are active surveillance, radiation therapy, and surgery to remove the prostate. Active surveillance may be recommended for slow-growing cancer that's confined to the prostate.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Cause
Experts don't know exactly what causes prostate cancer. But they do know that changes in the body's DNA are involved. These include DNA changes that are inherited as well as those that happen as you get older.
The prostate usually gets larger as you age. Having an enlarged prostate doesn't increase your chance of getting prostate cancer. But an enlarged prostate is sometimes caused by prostate cancer.
What Increases Your Risk
Some things can increase your chances of getting prostate cancer. These risk factors include:
- Age.
-
Getting older is the main risk factor for prostate cancer. Most cases occur after age 65.
- Family history.
-
Your chances of getting the disease are higher if someone in your family has had it. Your risk also depends on the age at which your relative was diagnosed.
- Race.
-
Prostate cancer is more common among African-American people than people of other races.
Lowering Your Risk
There are some risk factors for prostate cancer that you can't control, such as getting older or inheriting certain gene changes. But you may be able to help lower your risk for prostate cancer (and some other cancers) by staying at a healthy weight, being active, and not smoking.
Learn more
Symptoms
Prostate cancer usually doesn't cause symptoms in its early stages. Most people don't know they have it until it is found during a regular medical exam.
When there are symptoms of prostate cancer, they often include urinary problems, such as:
- Not being able to urinate at all.
- Having a hard time starting or stopping the flow of urine.
- Having to urinate often, especially at night.
- Feeling pain or burning during urination.
Less common symptoms may include:
- Difficulty having an erection.
- Blood in your urine or semen.
- Deep and frequent pain in your lower back, belly, hip, or pelvis.
What Happens
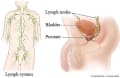
Prostate cancer usually grows slowly. It usually takes years to get large enough to cause any problems. But sometimes it grows quickly. When prostate cancer spreads beyond the prostate, it goes first to the lymph nodes in the pelvis, and then on to the bones, lungs, or other organs.
About 12 out of 100 men in the U.S. will be diagnosed with prostate cancer sometime during their lifetime.footnote 1 But most people who are diagnosed with prostate cancer don't die from it.
Progression of prostate cancer
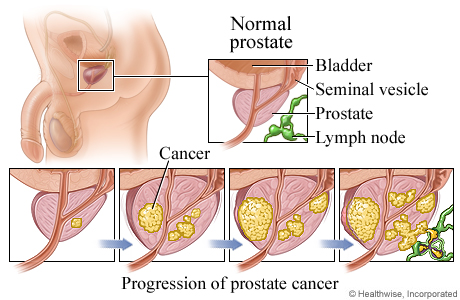
Prostate cancer begins inside the prostate gland. Usually this cancer grows so slowly that it may never cause a problem during a person's life. But in some cases, it grows more quickly, spreading into nearby tissues, such as the lymph nodes or seminal vesicles, and to other areas of the body.
Learn more
When to Call a Doctor
Call your doctor now if:
- You cannot urinate.
- You have symptoms of a urinary infection. For example:
- You have blood or pus in your urine.
- You have pain in your back just below your rib cage.
- You have a fever, chills, or body aches.
- It hurts to urinate.
- You have groin or belly pain.
- You have pain in your back or hips.
- Your pain isn't controlled.
- You are vomiting or nauseated.
Watch closely for changes in your health, and be sure to contact your doctor if:
- You have pain when you ejaculate.
- You have trouble starting or controlling your urine.
If you have been diagnosed with cancer, be sure to follow your doctor's instructions about calling when you have problems, new symptoms, or symptoms that get worse.
Exams and Tests
Your doctor will ask you about your family history and your medical history. You will have a physical examination that includes a digital rectal exam, in which the doctor inserts a gloved finger into your rectum to feel your prostate.
Tests that may be used to check for prostate cancer include:
- Blood tests, such as a prostate-specific antigen (PSA) test, a complete blood count (CBC), and a blood chemistry test.
- Imaging tests to check the prostate for cancer and to see if the cancer has spread outside the prostate. These tests may include:
- A CT scan.
- An MRI or a multiparametric MRI (mpMRI). An mpMRI shows a detailed image of the prostate tissue.
- A positron emission tomography (PET) scan, a PET-CT scan, or a PET-MRI.
- A bone scan.
- A transrectal ultrasound.
- A prostate biopsy. Tissue is taken from the prostate and examined under a microscope. A biopsy is the only way to confirm whether you have prostate cancer.
- Genetic tests, such as:
- Tests that check for any inherited gene changes, such as BRCA gene changes.
- Tests that check for biomarkers in prostate tissue from the biopsy sample. Some biomarker tests look for signs of cancer in a sample of blood or urine.
Screening tests for prostate cancer
The main screening test for prostate cancer is the prostate-specific antigen (PSA) test. It's a blood test that measures how much PSA is in your blood. And you will probably have a digital rectal exam. A high PSA level may mean that you have an enlarged prostate, an infection or, less often, prostate cancer.
The prostate-specific antigen (PSA) test can help find prostate cancer early. But experts recommend that you discuss the benefits and risks of the test with your doctor before you decide whether to have this test. It may not help you live any longer than if you had no screening. And it could lead to harmful treatments that you don't need.
Talk with your doctor about your health, your risk factors for prostate cancer, and the pros and cons of PSA testing.
Learn more
- Bone Scan
- Chemistry Screen
- Complete Blood Count (CBC)
- Computed Tomography (CT) Scan of the Body
- Digital Rectal Examination
- Magnetic Resonance Imaging (MRI)
- Pelvic Ultrasound
- Prostate Biopsy
- Prostate Cancer Screening
- Prostate Cancer Screening: Should I Have a PSA Test?
- Prostate-Specific Antigen (PSA) Test
Treatment Overview
Treatment for prostate cancer is based on the stage of the cancer, your Gleason score, and other things, such as your age and overall health. The main options are active surveillance, radiation therapy, and surgery to remove the prostate. Hormone therapy is sometimes given along with radiation therapy or surgery. Other treatments may be used, such as chemotherapy and immunotherapy.
Your doctor will talk with you about your options and then make a treatment plan. Some people choose watchful waiting instead of treatment.
Some people use complementary therapies along with traditional medical treatment. These therapies may help you cope with the symptoms and stress of cancer. For example, acupuncture may help reduce hot flashes caused by hormone therapy. Talk with your doctor about any of these options you would like to try.
Active surveillance
This may be an option if the cancer is slow-growing and confined to the prostate (localized). With active surveillance, you'll have regular checkups and tests, but you won't have treatment unless the cancer grows.
Treatments such as surgery or radiation can cause serious side effects. Active surveillance lets you avoid or postpone treatment and its side effects. Some people who have very slow-growing localized prostate cancer may never need treatment. Others can delay treatment until tests show that the cancer is growing more quickly.
If you choose this option, it's very important to follow your doctor's schedule of tests and exams. This increases the chance of finding out right away if the cancer starts growing. Then it can be treated in the early stages, when treatment is most successful.
Even if the cancer isn't growing, you can choose to start treatment at any time.
Radiation therapy
Radiation therapy uses high-dose X-rays to destroy cancer cells and shrink tumors. Radiation for prostate cancer is usually given by a machine outside the body (external radiation). It may also be given by placing substances inside the body (internal radiation, or brachytherapy).
Radiation therapy may be used alone to treat prostate cancer. Or it may be combined with hormone therapy if tests show that the cancer is likely to grow. Radiation is sometimes used after surgery to destroy any remaining cancer cells.
Surgery
Surgery to remove the prostate is called radical prostatectomy. This is most often done if tests show the cancer hasn't spread outside the prostate (localized cancer). A doctor removes the whole prostate and the seminal vesicles. The doctor also removes any nearby tissue that may contain cancer. This may be done as:
- Laparoscopic surgery.
- This is done through several very small cuts in the belly. The doctor uses a tiny camera and special tools. Most doctors do it by guiding robotic arms that hold the surgery tools. This is called robot-assisted prostatectomy.
- Open surgery.
- The doctor may do surgery through one cut (incision) in the belly. This is called the retropubic approach. Or it may be done through an incision between the anus and the scrotum (perineum). This is called the perineal approach.
If possible, the doctor will try to save the nerves that are needed for an erection. This can only be done when there is no chance of leaving cancer cells behind.
The doctor may also remove lymph nodes in the pelvic area to check them for cancer. This is called pelvic lymph node dissection.
Hormone therapy
Prostate cancer needs male sex hormones (androgens) to grow. Hormone therapy lowers the level of androgens in your body. This can slow the growth of prostate cancer and even shrink the tumors. This may also be called androgen deprivation therapy (ADT).
The main androgen is testosterone. It is mostly made by the testicles. Hormone therapy may be done with:
- Medicines.
- Hormone therapy is often done with medicines that block testosterone. These may be given as shots or pills.
- Surgery.
- Surgery may be done to remove the testicles (bilateral orchiectomy). This lowers the testosterone level right away.
Other treatments
Other treatments may be used, especially if prostate cancer has come back after treatment (recurrent cancer) or has spread to other parts of the body (metastatic cancer). Examples include:
- Chemotherapy.
- These medicines kill fast-growing cells, including cancer cells and some normal cells.
- Cryosurgery.
- This treatment uses extreme cold to destroy cancer cells.
- Immunotherapy.
- This treatment helps your immune system fight cancer. It may be given in several ways.
- Targeted therapy.
- These medicines target cancer cells and may cause less harm to normal cells. They help keep cancer from growing or spreading.
- High-intensity focused ultrasound (HIFU).
- This treatment uses sound waves to create heat that destroys cancer cells.
Watchful waiting
Watchful waiting is a wait-and-see approach to treatment that may be an option for certain people. You would have regular visits with your doctor but fewer tests than with active surveillance. The focus is on treating any symptoms that bother you rather than trying to cure the cancer. This may be a good choice if you are too ill to have (or don't want to have) aggressive treatment, such as surgery.
As with active surveillance, you can change your mind and start treatment at any time.
Learn more
- Active Surveillance for Prostate Cancer
- Cryosurgery for Prostate Cancer
- Hormone Therapy for Prostate Cancer (Androgen Deprivation Therapy, or ADT)
- Immunotherapy for Cancer
- Prostate Cancer: Should I Choose Active Surveillance?
- Prostate Cancer: Should I Have Radiation or Surgery for Localized Prostate Cancer?
- Radiation Therapy for Prostate Cancer
- Radical Prostatectomy
Supportive Care
Palliative care is a type of care for people who have a serious illness. It's different from care to cure your illness, called curative treatment. Palliative care provides an extra layer of support that can improve your quality of life—not just in your body, but also in your mind and spirit. Sometimes palliative care is combined with curative treatment.
The kind of care you get depends on what you need. Your goals guide your care. You can get both palliative care and care to treat your illness. You don't have to choose one or the other.
Palliative care can help you manage symptoms, pain, or side effects from treatment. It may help you and those close to you better understand your illness, talk more openly about your feelings, or decide what treatment you want or don't want. It can also help you communicate better with your doctors, nurses, family, and friends.
End-of-life care
It can be hard to live with an illness that cannot be cured. But if your health is getting worse, you may want to make decisions about end-of-life care. Planning for the end of your life does not mean that you are giving up. It is a way to make sure that your wishes are met. Clearly stating your wishes can make it easier for your loved ones. Making plans while you are still able may also ease your mind and make your final days less stressful and more meaningful.
Learn more
Self-Care
- Take your medicines exactly as prescribed. Call your doctor if you think you are having a problem with your medicine.
- Follow your doctor's instructions to relieve pain. Pain from cancer and surgery can almost always be controlled. Use pain medicine when you first notice pain, before it becomes severe.
- Eat healthy food. If you do not feel like eating, try to eat food that has protein and extra calories to keep up your strength and prevent weight loss.
- Get some physical activity every day, but do not get too tired.
- Get enough sleep, and take time to do things you enjoy. This can help reduce stress.
- Think about joining a support group. Or discuss your concerns with your doctor or a counselor.
- If you are vomiting or have diarrhea:
- Drink plenty of fluids to prevent dehydration. Choose water and other clear liquids. If you have kidney, heart, or liver disease and have to limit fluids, talk with your doctor before you increase the amount of fluids you drink.
- When you are able to eat, try clear soups, mild foods, and liquids until all symptoms are gone for 12 to 48 hours. Jell-O, dry toast, crackers, and cooked cereal are also good choices.
- If you have not already done so, prepare a list of advance directives. Advance directives are instructions to your doctor and family members about what kind of care you want if you become unable to speak or express yourself.
Learn more
- Cancer: Controlling Cancer Pain
- Cancer: Controlling Nausea and Vomiting From Chemotherapy
- Cancer: Home Treatment for Constipation
- Cancer: Home Treatment for Diarrhea
- Cancer: Home Treatment for Fatigue
- Cancer: Home Treatment for Mouth Sores
- Cancer: Home Treatment for Pain
- Cancer: Home Treatment for Sleep Problems
- Cancer Support: Managing Stress
- Eating Well During Cancer Treatment
- Hair Loss From Cancer Treatment
Complementary Treatments
Some people use complementary therapies along with medical treatment. They may help relieve the symptoms and stress of cancer or the side effects of cancer treatment. Therapies that may be helpful include:
- Acupuncture to relieve pain and other symptoms.
- Meditation or yoga to relieve stress.
- Massage and biofeedback to reduce pain and tension.
- Breathing exercises to help you relax.
Talk with your doctor about any of these options you would like to try. And let your doctor know if you are already using any complementary therapies. They are not meant to take the place of standard medical treatment. But they may help you feel better and cope better with treatment.
Learn more
Getting Support
Relationships take on new importance when you're faced with cancer. Your family and friends can help support you. You may also want to look beyond those who are close to you.
- Reach out to your family and friends.
Remember that the people around you want to support you, and asking for help isn't a sign of weakness.
- Tell them how they can help.
Your friends and family want to help, but some of them may not know what to do. It may help to make a list. For example, you might ask them to:
- Run errands or pick up kids.
- Deliver meals or groceries to your home.
- Drive you to appointments.
- Go to doctor visits with you and take notes.
- Look for help from other sources.
Places to turn for support include:
- Counseling.
- Counseling can help you cope with cancer and the effect cancer is having on your life. Different types of counseling include family therapy, couples therapy, group counseling, and individual counseling.
- Your health care team.
- Your team should be supportive. Be open and honest about your fears and concerns. Your doctor can help you get the right medical treatments, including counseling.
- Spiritual or religious groups.
- These groups can provide comfort and may be able to help you find counseling or other social support services.
- Social groups.
- Social groups can help you meet new people and get involved in activities you enjoy. Focus on activities that bring you comfort, such as spending time outdoors or being with children.
- A cancer support group.
- Cancer support groups offer support and practical advice. You can hear others talk about:
- What it's like to live with cancer.
- Practical ways to manage your cancer treatment and its side effects.
- Ways to cope with your illness.
Learn more
Related Information
References
Citations
Credits
Current as of: October 25, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 25, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use and Privacy Policy. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2025 Ignite Healthwise, LLC.